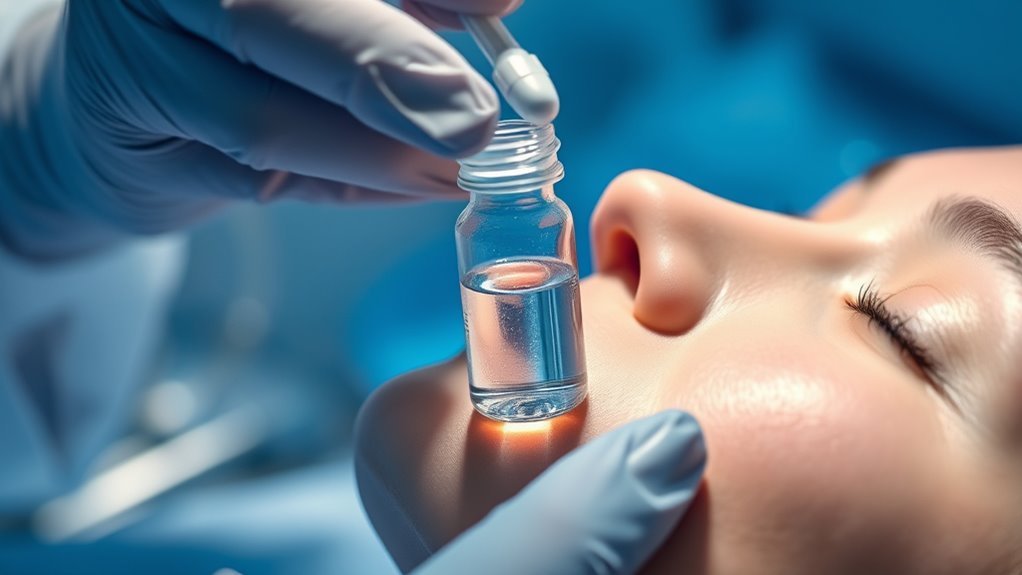
Exosome therapy in skin rejuvenation delivers bioactive signals—proteins, lipids, and nucleic acids—from donor cells to your skin, modulating inflammation, collagen remodeling, and pigmentation. Mechanisms include paracrine signaling that supports extracellular matrix turnover and targeted cargo that can rebalance tone. Delivery method matters: topical applications offer accessibility but variable absorption, while intradermal approaches permit higher, controlled exposure. Expect gradual improvements over months, with procedure-specific risks and the need for standardized sourcing, informed consent, and real maintenance plans as you weigh options. More specifics await.
Understand Exosomes: What They Are and How They Help Skin
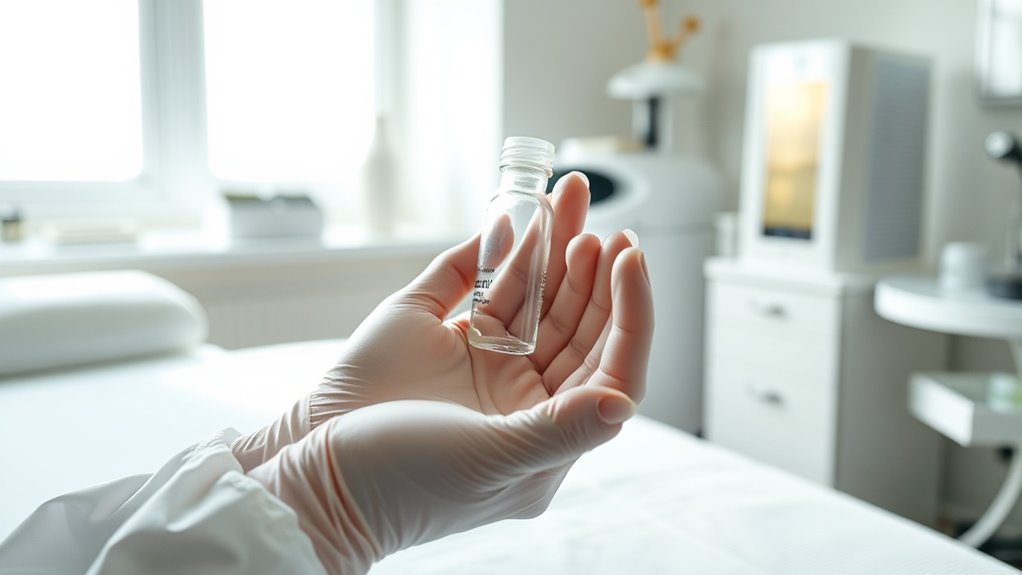
Exosomes are tiny vesicles released by cells that carry proteins, lipids, and nucleic acids, and they play a key role in intercellular communication. You’ll learn that these vesicles reflect their cell of origin and influence recipient cells by transferring cargo that modulates signaling pathways and gene expression. In skin, exosomes contribute to processes like collagen synthesis, pigmentation, and inflammation resolution, offering a biologically plausible route for restorative effects. Mechanistically, their cargo includes microRNAs and growth factors that can alter fibroblast activity and extracellular matrix remodeling. When considering therapies, exosome sourcing and regulatory approval are critical: you should seek transparent, quality-assured products with robust characterization and clear standards. This positions you to evaluate options confidently and join a community pursuing safe, evidence-based skin rejuvenation.
How Exosome Therapy Works: Mechanisms for Brightening and Rejuvenation
Building on what we know about exosomes’ role in skin biology, this section explains how their cargo translates into brighter, younger-looking skin. You’ll learn that exosome contents—growth factors, miRNAs, and proteomic signals—modulate inflammation, stimulate collagen, and enhance melanocyte regulation, collectively supporting visible luminance and texture. Mechanistically, paracrine signaling improves extracellular matrix remodeling and cellular turnover, while targeted delivery can rebalance pigmentation pathways. You’ll encounter variability based on source material and preparation, underscoring the need for rigorous standardization. Exosome sourcing, donor screening, and processing practices influence safety and consistency, shaping outcomes you may expect. Ethical considerations matter: transparency about origins, consent, and proprietary methods helps you assess value and trust in therapy. Informed choices rely on precise, evidence-based discipline.
Exosome Delivery Methods for Skin: Pros, Cons, and What to Expect

Topical and intradermal delivery each offer distinct accessibility and penetration profiles you should weigh against safety and practical use. While topical applications are convenient, their transdermal absorption can be limited and variable, whereas intradermal delivery targets deeper layers but may require professional administration and carry laser-focused safety considerations. Across both methods, assess documented efficacy, potential adverse effects, and what to expect in terms of onset, duration, and need for follow-up.
Topical vs. Intradermal Delivery
Which delivery method suits skin rejuvenation goals better: topical applications or intradermal injections? You weigh mechanisms, evidence, and practicality. Topical exosome formulations rely on permeation enhancers and microneedling adjuncts to boost penetration, but variability in barrier function creates a topic mismatch that can limit consistency. Intradermal injections deliver cells and signals directly into the dermis, offering more controlled exposure and rapid microenvironment modulation, yet they require clinician administration and carry greater procedural risk. Overall, topical options favor gradual, accessible upkeep, while intradermal methods align with targeted improvements and higher-dose delivery. Your choice should reflect skin type, goals, and tolerance for procedures, acknowledging that evidence remains evolving and unrelated focus of outcomes may arise if expectations aren’t aligned with delivery realities.
Safety, Efficacy Considerations
When evaluating safety and efficacy of exosome delivery for skin, you’ll weigh how each method shapes exposure, risk, and outcomes. Delivery method influences particle integrity, dosing consistency, and potential immune reactions, so you assess exosome sourcing, production quality, and documented adverse events. Topical and intradermal approaches offer distinct exposure profiles: surface application reduces invasiveness but may limit penetrance, while injections boost dermal delivery but raise transient discomfort and risk of local reactions. Evidence suggests modest, variable improvements in texture and tone, with outcome durability differing by product and technique. Ethical considerations, regulatory status, and standardized potency assays matter for trust and reproducibility. Align expectations with available data, monitor responses closely, and prioritize transparent discussions about each option’s benefits, limitations, and safety profile.
What Happens During an Exosome Treatment: Steps, Pain, and Downtime
Exosome treatments typically involve a brief, office-based procedure. You’ll start with a consultation, then a topical anesthetic or nerve block may be applied to minimize discomfort. The actual delivery uses microneedling, injection, or infusion, depending on your dermatologist’s protocol and the product’s formulation. Pain is typically mild to moderate and episodic, managed with local anesthetic options and cooled devices. Downtime ranges from none to a few days, with transient redness, swelling, or pinpoint itching that usually resolves quickly. Expect slight tenderness as you recover. When you plan, consider that regimens vary by product and practice; ensure/guarantee your provider can discuss exosome sourcing and the regulatory approval status of the preparation used. This transparency supports informed decisions and a sense of trust.
Realistic Results: Timelines and What You’ll See First

You’ll typically notice initial improvements within a few days to weeks as early skin texture and hydration respond to exosome therapy. Over the next several weeks, visible changes—such as tone, pore appearance, and radiance—often align with the Initial Improvements Timeline and Visible Changes Timeline. Long-Term Outcome Milestones describe what sustained results look like over months, helping you gauge durability and plan any follow-up treatments.
Initial Improvements Timeline
What sort of improvements should you expect after exosome therapy for skin rejuvenation, and on what timeline do they typically appear? In the initial weeks, you may notice subtle texture refinement, slight pore smoothing, and a more even tone as micro-inflammatory processes promote collagen signaling. Changes are gradual, not dramatic, harmonizing with evidence that early cellular responses precede visible remodeling. You’ll gauge progress through patient-reported texture improvements and clinician assessments rather than instantaneous radiance gains. Critical factors include consistent treatment intervals and adherence to post-care guidance. Quality controls—such as exosome sourcing and strict cold chain management—support predictable outcomes. While individual timelines vary, most early gains emerge within 2–6 weeks, with continued refinement as remodeling proceeds over subsequent months.
Visible Changes Timeline
How soon will you notice visible changes after an exosome therapy session, and what should you expect first? You’ll see subtle tonal improvements and texture refinement within days, with more defined lift and glow over weeks. Evidence-based progress follows a logical pattern: initial micro-edema subsides, collagen remodeling begins, and pigment harmonizes, all contributing to a smoother canvas. This timeline aligns with typical tissue repair dynamics, not instantaneous overhaul, and it emphasizes tone alignment and natural results. Below, a concise grid highlights expected milestones while keeping you connected to the process.
| Milestone | Timeframe | Expected Effect |
|---|---|---|
| Early texture smoothing | 1–2 weeks | Softer skin feel, less roughness |
| Tone refinement | 2–4 weeks | More even complexion, glow |
| Subtle lift signals | 4–8 weeks | Fewer fine lines, enhanced clarity |
Long-Term Outcome Milestones
Long-term results from exosome therapy reflect cumulative tissue remodeling rather than immediate changes. You’ll notice gradual improvements as collagen structure adapts and inflammation settles, with peak effects unfolding over months. Realistic timelines depend on product quality, including exosome sourcing, and your individual skin biology, but some milestones are common.
- Gradual texture refinement begins weeks after treatment
- Subtle pore reduction and tone evening within 1–3 months
- Fine lines soften with continued remodeling over 3–6 months
- Dermal elasticity improvements emerge after multiple sessions
- Sustained results rely on ongoing maintenance and regulatory approval of the therapy
Keep in mind, enduring outcomes hinge on consistent follow-ups, adherence to aftercare, and verified regulatory approval to ensure safety and efficacy.
Safety First: Risks, Side Effects, and How to Minimize Them
Exosome therapies for skin rejuvenation carry potential benefits, but they also pose safety considerations that require careful management. You should understand that risks include local reactions, infection, and variability in product quality, which can influence outcomes. Side effects are usually mild but can extend to swelling, redness, or tenderness at the injection site, and less commonly, hypersensitivity. To minimize harm, choose regulated providers, confirm traceability of exosome sources, and review manufacturing standards aligned with industry guidelines. Adhere to conservative treatment plans, document adverse events, and seek informed consent that covers uncertainties. An informed patient community thrives when open dialogue exists, including ongoing ethics debate and transparent safety reporting. Your diligence supports reliable care and aligns with evidence-based practice.
Who Should Consider Exosome Therapy: Candidate Criteria
You are an ideal candidate if you’re considering non-surgical rejuvenation and have realistic expectations about outcomes. Your medical history matters—active infections, certain autoimmune conditions, or anticoagulant use may affect suitability, although well-controlled chronic conditions are more compatible with treatment. Key criteria include overall skin health, prior procedures, and a candidacy assessment that weighs the potential benefits against risks.
Ideal Candidate Profile
Ideal candidates are adults with signs of aging or skin quality concerns that respond to growth factor–mediated signaling but who don’t have contraindicating conditions.
- You seek improvements in texture, tone, and subtle volume loss with a non-surgical approach
- You understand that results depend on exosome sourcing and product quality
- You have realistic expectations about gradual, incremental changes
- You’re committed to pursuing evidence-based options within regulatory approvals
- You value guidance from clinicians who tailor protocols to your skin biology
These criteria support informed decision-making, aligning therapy with safety standards and proven mechanisms. If you don’t meet these conditions, consider alternative rejuvenation strategies. Your participation hinges on clear consent, transparent discussion of benefits, and adherence to approved applications within regulatory approvals.
Medical History Considerations
Medical history is critical to determine suitability for exosome therapy, balancing potential skin benefits against systemic risks and prior treatments. You should review chronic illnesses, autoimmune conditions, and current medications that affect healing or bleeding. Prior cosmetic procedures, recent infections, and active dermatologic disease can influence outcomes and safety. Your clinician will assess analgesic use, anticoagulants, immunosuppressants, and diabetes control, as these factors shape infection risk and recovery. Consider lifestyle factors, including smoking and sun exposure, which may impact results. Discuss exosome sourcing and any prior exposure to biologic products, as these influence immunologic response and regulatory approval pathways. A comprehensive history enables personalized risk–benefit appraisal, helping you decide whether pursuing exosome therapy aligns with your goals and safety profile.
Treatment Suitability Criteria
When evaluating treatment suitability, consider who may benefit from exosome therapy based on objective skin concerns, health status, and prior responses to other interventions.
- Objective concerns align with particle size, pigmentation, texture, or scarring patterns
- Health status includes immune considerations, systemic diseases, and medications that affect healing
- Prior responses to microneedling, lasers, or topical therapies inform likely benefit
- Informed expectations address realistic timelines and possible need for maintenance
- Practical factors cover access to providers, exosome sourcing, and regulatory status
This framework supports a precise, evidence-based decision, fostering belonging through shared decision-making. You’ll weigh exosome sourcing implications and regulatory status, ensuring safety, transparency, and alignment with personal goals.
Compare Costs and Insurance: What It Takes to Budget
How much will exosome therapy for skin rejuvenation cost, and how can you maneuver insurance coverage? You’ll find costs vary by provider, location, treatment plan, and number of sessions, making a solid cost comparison essential. Generally, per-session prices range widely, so you should request itemized quotes and confirm what’s included (consultation, injection, follow-ups). Many plans don’t cover aesthetic procedures, but some clinics offer financing or bundles that reduce the per-session rate. Approach coverage with documentation: explain medically framed goals, request preauthorization if applicable, and verify any patient-assisted discounts. Track total expenditure across potential providers, factoring travel costs and downtime. By assembling a transparent budget, you’ll know your true investment and align choices with your aesthetic goals and insurance coverage.
Maintaining Results: How Exosomes Fit Into a Skincare Regimen
Maintaining results from exosome therapy hinges on consistency and integration with a broader skincare plan. You should view exosome use as one component within an evidence-based routine that emphasizes protection, renewal, and measured optimization. Regular, targeted applications align with your skin’s natural cycles and can sustain improvements when combined with proven practices. Key factors include product quality, sourcing transparency, and adherence to safety guidelines governed by regulatory oversight. Monitor skin response and adjust timing with professional guidance to avoid diminishing returns.
- exosome sourcing transparency and product provenance
- consistent sun protection and antioxidant support
- nonirritating cleansers and fragrance-free formulations
- periodic professional evaluation to recalibrate regimen
- clear documentation of results and any adverse reactions
Questions to Ask Your Clinician Before Proceeding
Before you proceed, it’s crucial to go into your consultation with clear, targeted questions that help you assess safety, efficacy, and fit for your goals. You’ll want concrete answers about exosome supply, including sourcing standards, processing methods, and lot traceability. Ask how outcomes are measured, the evidence supporting claims, and expected timelines for visible results. Probe potential risks, allergy history, and post-treatment care. Request credentials, clinic accreditation, and the clinician’s experience with your skin type. Be wary of marketing hype and unsolicited guarantees. Discuss alternative options, maintenance plans, and cost transparency. Seek written informed consent detailing product specifics, anticipated benefits, and risks. A thoughtful dialogue grounds your decision in verifiable data and shared decision-making, reinforcing a sense of belonging to a safe, evidence-driven care community.
Frequently Asked Questions
Are Exosomes Fda-Approved for Cosmetic Skin Use?
No. Exosome products aren’t FDA-approved for cosmetic skin use, and you should treat unapproved claims cautiously. The FDA hasn’t granted clearance or labeling for these therapies, so regulatory oversight remains unclear. When assessing options, review FDA status and seek products backed by safety data from reputable trials. You deserve transparent, evidence-based guidance, so ask providers about safety data, potential risks, and post-treatment monitoring before proceeding.
How Long Do Exosome Treatments Last on Average?
Exosome treatments typically last several weeks to a few months, with average duration around 4–6 weeks for noticeable effects. Individual results vary by skin type, aging, and maintenance routines. To optimize exosome duration, you may pursue follow-up sessions every 4–8 weeks, coordinating with treatment longevity data. Although not universally permanent, consistent scheduling can sustain improvements longer. You’ll feel more confident knowing you’re supported by evidence-based approaches and a community that shares similar goals.
Can Exosome Therapy Replace Lasers or Fillers?
Exosome therapy can’t reliably replace lasers or fillers. Consider a hypothetical patient who combines mild exosome treatments with laser resurfacing to improve texture and collagen; the combination can offer complementary benefits, not a substitute. You should review exosome sourcing and current regulatory status before pursuing any plan. Evidence varies, and regulatory status differs by region, influencing safety and claims. You’ll want clear data on indications, timelines, and realistic outcomes to decide if it fits your goals.
Do Exosome Products Require Prescription or Clinic-Only Use?
Yes, exosome products are typically clinic-only or require a prescription, depending on local regulations and product type. You’ll usually access them through licensed practitioners who assess eligibility and supervise treatment. Consider factors like exosome sourcing quality and batch consistency, and discuss recommended treatment frequency with your clinician. Evidence supports gradual, individualized plans rather than one-size-fits-all, so you’ll want to cooperate with a provider who emphasizes transparency, safety, and ongoing monitoring for optimal results.
Are There Any Long-Term Safety Concerns With Repeated Sessions?
There can be concerns about long term risks with repeated sessions. Current evidence suggests exosome therapies are generally well tolerated, but data on extended, repeated use remains limited. You should monitor for cumulative effects, sensation changes, or unexpected reactions, and discuss with your clinician how often you’ll need sessions. If you pursue multiple treatments, ensure you’re in a regulated setting and that product quality, batch consistency, and informed consent are clearly addressed.